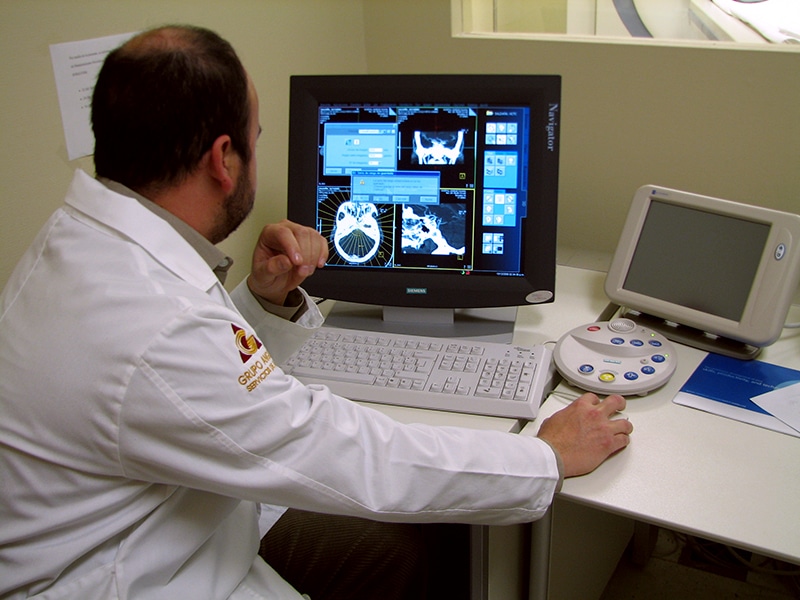
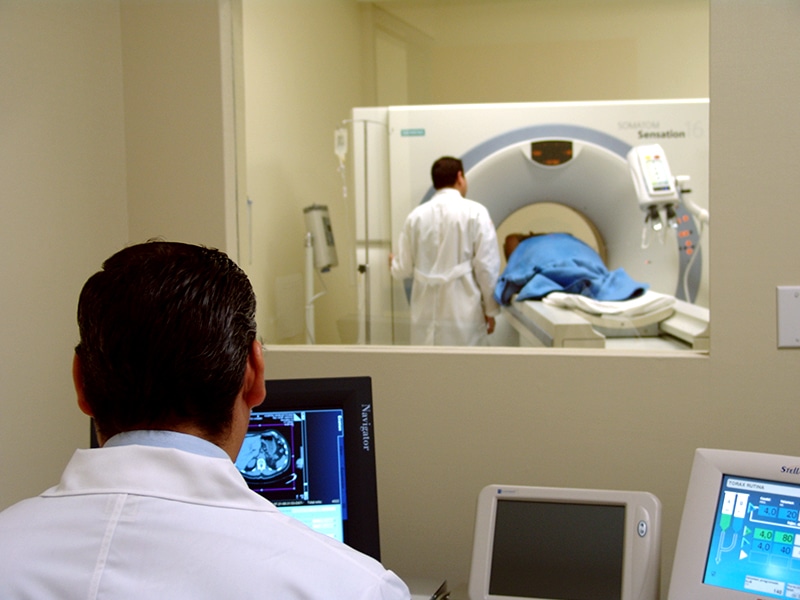
Custom Wavefront LASIK Surgery
Our Price: $ 3,900 USD
Wavefront LASIK surgery in a U.S. clinic can cost up to $5500 for each eye, depending on the location and the experience of the surgeon performing the procedure. The average cost for personalized LASIK at our hospital is $3,500 for both eyes, though cost may change according to individual patient characteristics.
While the invention of the Excimer laser made possible significant advances in the accuracy and ease of vision correction surgery based on the principles of radial keratotomy, recent developments in technology used to map the eye’s topography have taken standard LASIK surgery to new heights with a procedure known as Wavefront-guided LASIK.
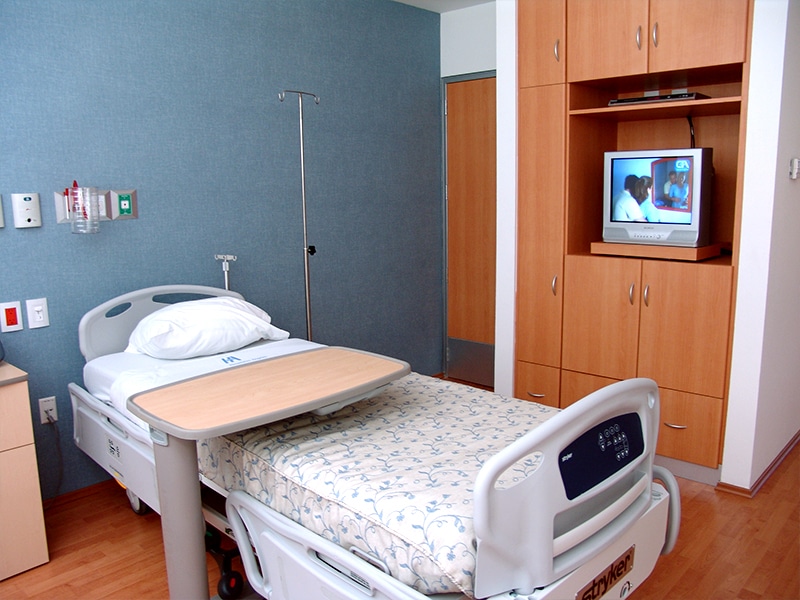
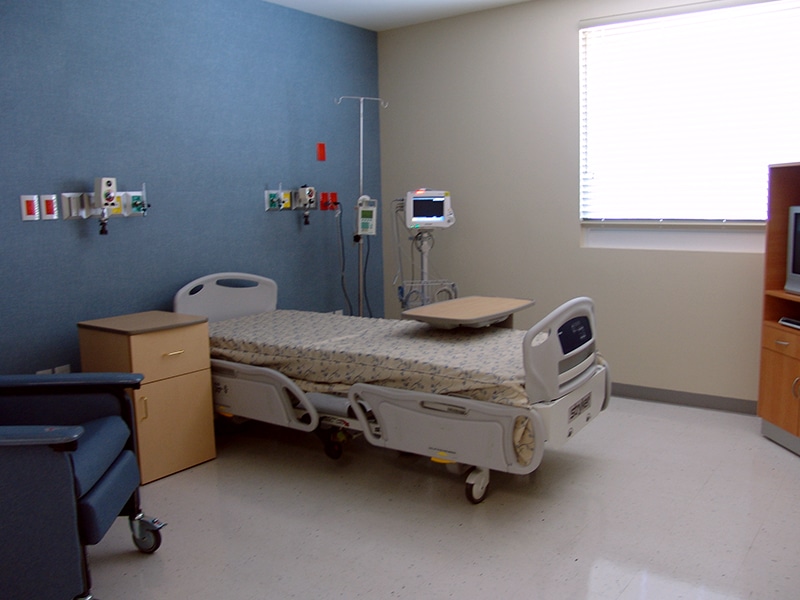
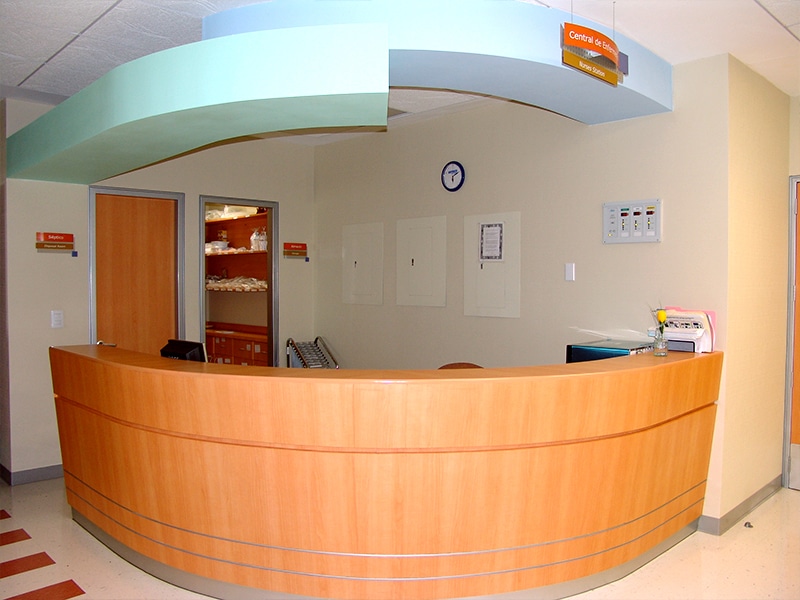
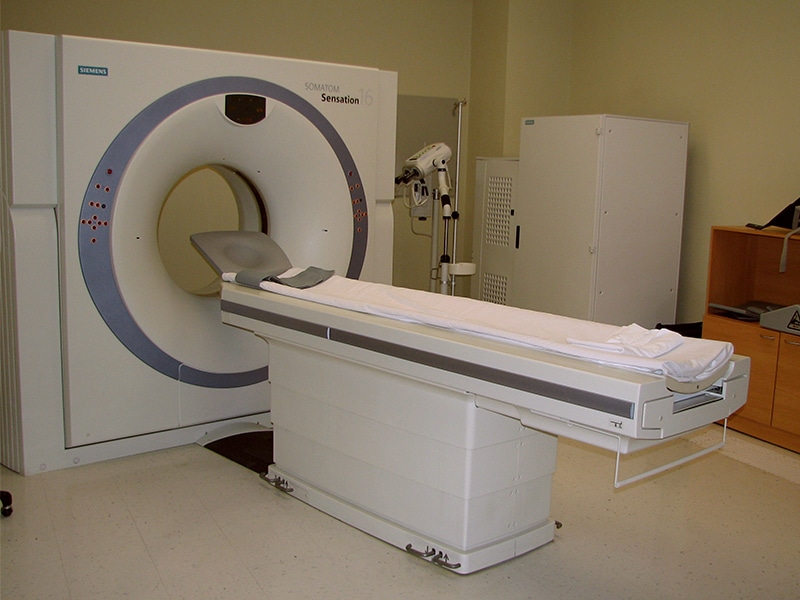
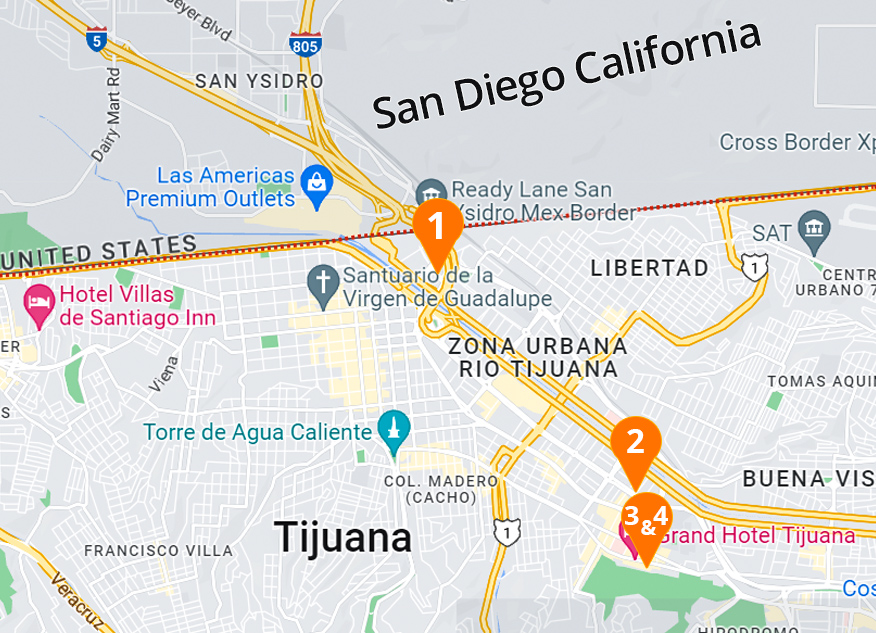
Angeles Hospital Facilities in Tijuana
Most Trusted and Recognized Hospital for +10 years
- Personalized attention with US based case manager
- Peace of mind of knowing you are getting treated by the highest quality and most prestigious hospital in Mexico
- Most recognized and trusted private medical institution in Mexico with over 10 years
- Fully equipped hospital with emergency rooms and 24hr. nurses for any type of unexpected situation (Not a Clinic like most)
- Best medical facilities in Tijuana
- Shuttle Service
- Many amenities
- Comfortable rooms with companion accommodations
Custom Wavefront LASIK Eye Surgery
Eye Vision Center of Excellence
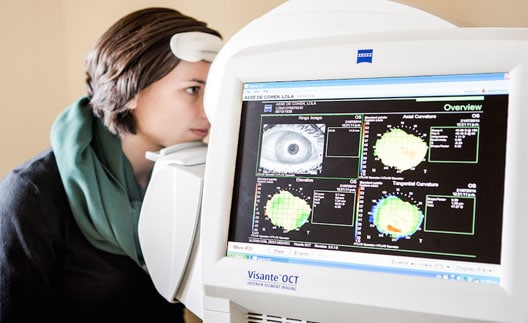
Also known as Wavefront LASIK or Custom LASIK, the procedure uses state-of-the-art laser mapping technology to measure the eye from front to back to create a three-dimensional (3-D) image, or “Wavefront” map, which a surgeon uses to guide the Excimer laser in customizing treatment for any individual’s unique visual system. Standard LASIK has been effective in treating lower-order aberrations (refractive errors) that result in nearsightedness, farsightedness and astigmatism, but not until the development of Wavefront cornea mapping technology did it become possible to treat higher-order aberrations responsible for such problems as decreased contrast sensitivity or night vision, glare, shadows and halos.
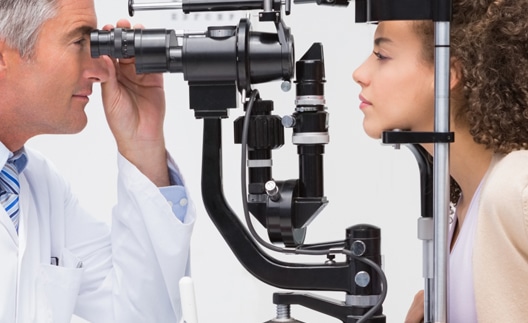
Custom Wavefront LASIK Eye Surgery
Eye Vision Center of Excellence
While higher-order aberrations do not affect vision in all cases, many LASIK patients in recent years have reported improvements in visual acuity measured in terms of contrast sensitivity and fine vision after undergoing Wavefront-guided LASIK procedures. Because Wavefront LASIK surgery or Custom LASIK has only been available in the US since 2001, there is little rigorously produced clinical data on the effectiveness or the long-term results of the procedure. However, several surveys have indicated as much as 94% of Custom LASIK patients report not only satisfaction with the results of the procedure, but also claim to be able to see as well as or better than they did with their corrective prescriptions before surgery. On the LASIK team we have Dr. Gabriel Carpio, who has a sub-specialty in Cornea and Refractive Surgery from the Institute of Ambulatory Surgery, as well as many other medical staff experienced in Wavefront LASIK surgery.